Fertility care has a timing problem. Not in the biological sense, though that matters, too, but in the way the system itself is structured. Most people enter fertility care too late. Not because they waited too long - but because it wasn’t clear how or where to get support sooner.
Consider the woman who spent years managing painful periods, told it was normal, never knowing endometriosis was quietly affecting her fertility. Or the person with PCOS who finally saw a specialist, only to be handed a referral for IVF before anyone explored what else might work. By the time most people get real answers about why they're struggling to conceive, they've already spent months - sometimes years - in uncertainty, bouncing between providers, searching for information online, and often landing in the most expensive treatment available simply because no one caught the signals earlier.
This isn't a failure of any single doctor, clinic, or patient. It's a structural one. Fertility care today is fragmented, reactive, and built on incomplete information. Testing happens in isolated snapshots. Care decisions are made without a full picture. And the result isn't just a difficult experience for families, it's billions of dollars in avoidable spend for the employers and payers trying to support them.

About 1 in 3 infertility patients discontinue treatment entirely, often without clear next steps. And many families spend $40,000–$70,000 to achieve pregnancy through IVF, often across multiple cycles.
We’ve been building toward a fundamentally different model, and it’s already delivering measurable results. Today, Maven’s model reduces total cost of care by roughly $9,600 per birth. A Fortune 100 bank working with Maven saw 15% lower total cost of care - a direct result of members getting the right care, in the right order, with the right support at every step.
Now we’re taking the next step. We’re introducing the first chapter of a new fertility model at Maven - one that starts earlier, with clinical understanding and guided pathways, so members reach the right outcome without defaulting to treatment.
Starting With What's Actually Happening in the Body
For too long, fertility care has begun at the point of crisis, when someone has already been trying for months, or years, and is ready for intervention. What often gets skipped is the diagnostic work that could have changed the trajectory entirely. Conditions like PCOS, endometriosis, or anovulation are remarkably common drivers of infertility, yet many people reach an IVF clinic without ever having them properly identified.
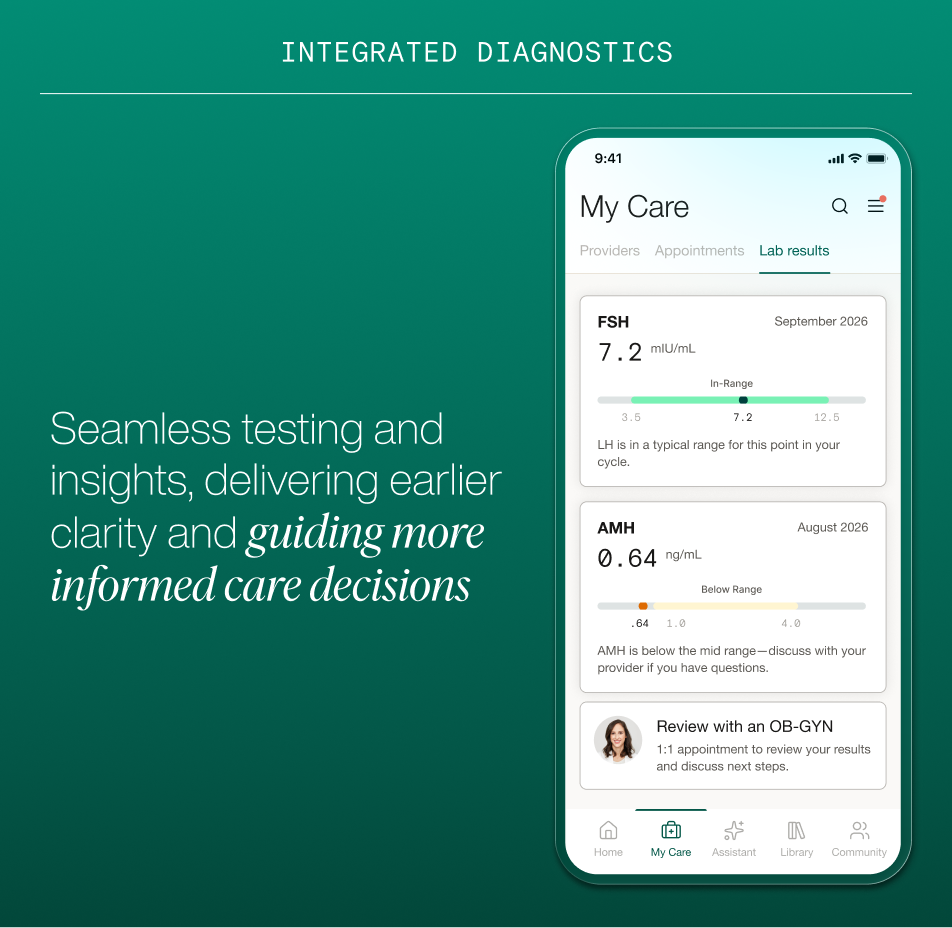
That's changing. Maven is now integrating diagnostics, lab work and continuous biometric data, directly into the care experience. Rather than treating testing as a one-time event that happens somewhere else, we're making it a continuous thread woven through every stage of a member's fertility journey.
This includes a first-of-its-kind partnership with Oura, bringing their FDA-regulated cycle prediction insights into a fertility care experience. This isn't wellness tracking. It's clinically validated data that helps surface ovulatory patterns and irregularities in real time, giving both members and their care teams a more complete view of what's happening between clinic visits.
The question isn't whether someone needs treatment, it's whether they've had a real chance to understand what's driving their fertility challenge before that treatment begins.
When you pair continuous wearable data with structured lab diagnostics, something shifts. Fertility stops being a guessing game and starts becoming visible earlier, and with more detail than a single office visit could ever provide.
From Data to Decisions
Data alone isn't the answer. What matters is what happens with it. One of the patterns we've seen repeatedly in fertility care is that even when members get testing done, the results don't meaningfully change the path they're on. They're handed lab values without context, or told to "keep trying" without a structured plan.
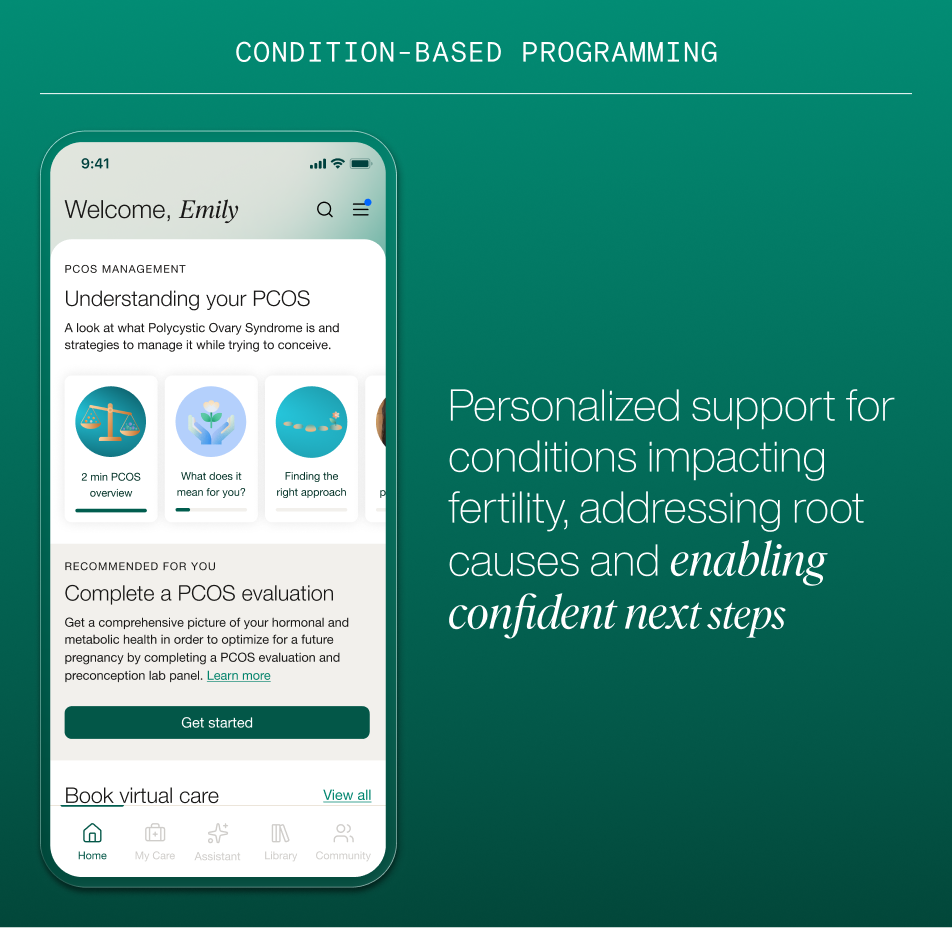
Maven's new condition-based care pathways are designed to close that gap. When diagnostics surface a specific fertility condition, PCOS, endometriosis, male factor infertility, or others, members don't just receive a label. They're guided into programming built around that condition: clinical recommendations, provider matching, lifestyle guidance, and a structured view of what the next steps actually look like.
This is the difference between giving someone information and giving them a path forward.
For employers, this matters for a very practical reason. When members receive the right guidance earlier, when the simplest, least invasive options are explored first, in the right order, the number of avoidable high-cost treatment cycles drops. Over the past decade, IVF efficiency per cycle has declined by more than 20%, even as utilization has climbed - suggesting that a meaningful share of cycles are adding cost without improving the odds. Better sequencing doesn't mean avoiding IVF. It means getting there only when it's the right next step.
One Experience, Not Twenty Touchpoints
Even with better diagnostics and smarter pathways, fragmentation remains the most persistent problem in fertility. Members today navigate between benefit portals, clinic systems, lab results from different providers, and mental health support that rarely talks to any of it. Every transition is a crack where people fall through.
What we're building is a connected fertility experience, one where diagnostics, care navigation, provider interactions, and clinical guidance all live in the same place. A member doesn't get a lab result in one app, a care plan in another, and emotional support in a third. It's one continuous journey, with each step informed by what came before it.
- Connected Diagnostics — Earlier visibility into what's happening. Lab work and continuous wearable data integrated into care, not siloed in a separate portal, so fertility signals surface sooner and inform every conversation.
- Guided Pathways — Care that matches the actual problem. Condition-based programming built around root causes like PCOS and endometriosis, so members get structured guidance, not generic advice.
- Connected Experience — One journey, not twenty fragments. Data, navigation, and clinical guidance in a single experience, so nothing gets lost between visits, providers, or life stages.
This matters for members, who no longer have to repeat their story or restart from scratch every time they see a new provider. And it matters for employers and payers who need a system that produces more consistent, predictable results, not just a benefit that reimburses whatever treatment happens next.
This Is the Beginning
We want to be transparent about what today's announcement represents. This is not the finished state of Maven's fertility model, it's the foundation.
What we're introducing now, connected diagnostics, condition-based pathways, and a more unified care experience, is the first step toward something more ambitious: a continuously improving fertility system. One where longitudinal data flows to the care teams who need it, where insights from similar member journeys help guide decisions, and where the system itself gets smarter over time as more data informs better outcomes.
That means clinic integration, shared records, and eventually, cohort-based insights that help set expectations and improve treatment decisions based on real-world patterns, not just individual anecdotes.
We're building this because the fertility industry needs - and the millions of families navigating fertility challenges deserve - something structurally different. Not a better reimbursement model or a shinier app. A system that seamlessly connects data, care, and decisions to transform how fertility care works for every person navigating it, and every organization working to support them. It's grounded in a simple idea: earlier information creates more options. More options create better outcomes. That's not a feature. That's a fundamentally different system.
Fertility care shouldn't begin at the point of crisis. It should begin at the point of clarity.
Join us to learn more
Sign up for our upcoming Fertility Roadmap Webinar to see these innovations in action and hear directly from Maven’s product and clinical leaders about what’s next for our maternity platform. Register here.
Ready to get started with Maven?
See how Maven can support working families, retain talent, and reduce costs



.png)


.jpg)

.jpg)
.png)

.jpg)
.png)
.jpeg)
.png)
