What you need to know:
New research shows that employers are adding more benefits programs, but employees aren’t feeling the support. The gap isn’t about the quantity of benefits—it’s about whether benefits are usable, visible, and trusted.
- Employers report increasing fertility, adoption, surrogacy, parenting, and midlife support year over year
- However, fewer employees say their benefits support them “very well” compared to last year
- Communication, navigation, and care coordination are now as important as coverage
- Employers who close this gap with end-to-end solutions can improve trust, engagement, and health outcomes
Employers are investing more in women’s and family health benefits than ever before. Over the past year, organizations have expanded fertility support, adoption and surrogacy assistance, paid parental leave, and parenting resources at meaningful rates, with further increases planned.
These investments reflect growing recognition that family health is central to workforce well-being and retention, a trend highlighted in Maven’s State of Women’s and Family Health Benefits 2026 report. Based on large-scale surveys of employees and benefits decision-makers across multiple markets, the report offers a dual perspective on how access, quality and trust are reshaping benefit offerings. The insights explored throughout this article are grounded in that data.
But many employees are not feeling the impact. Even as the number of offerings increase, fewer employees say their benefits support them “very well” across key areas of family building and women’s health when compared to last year. This disconnect signals a deeper issue in how benefits are delivered and experienced.
The challenge for 2026 is no longer just what benefits are offered, but whether employees can access and use them when it matters most.
Why do employees feel less supported even as benefits increase?
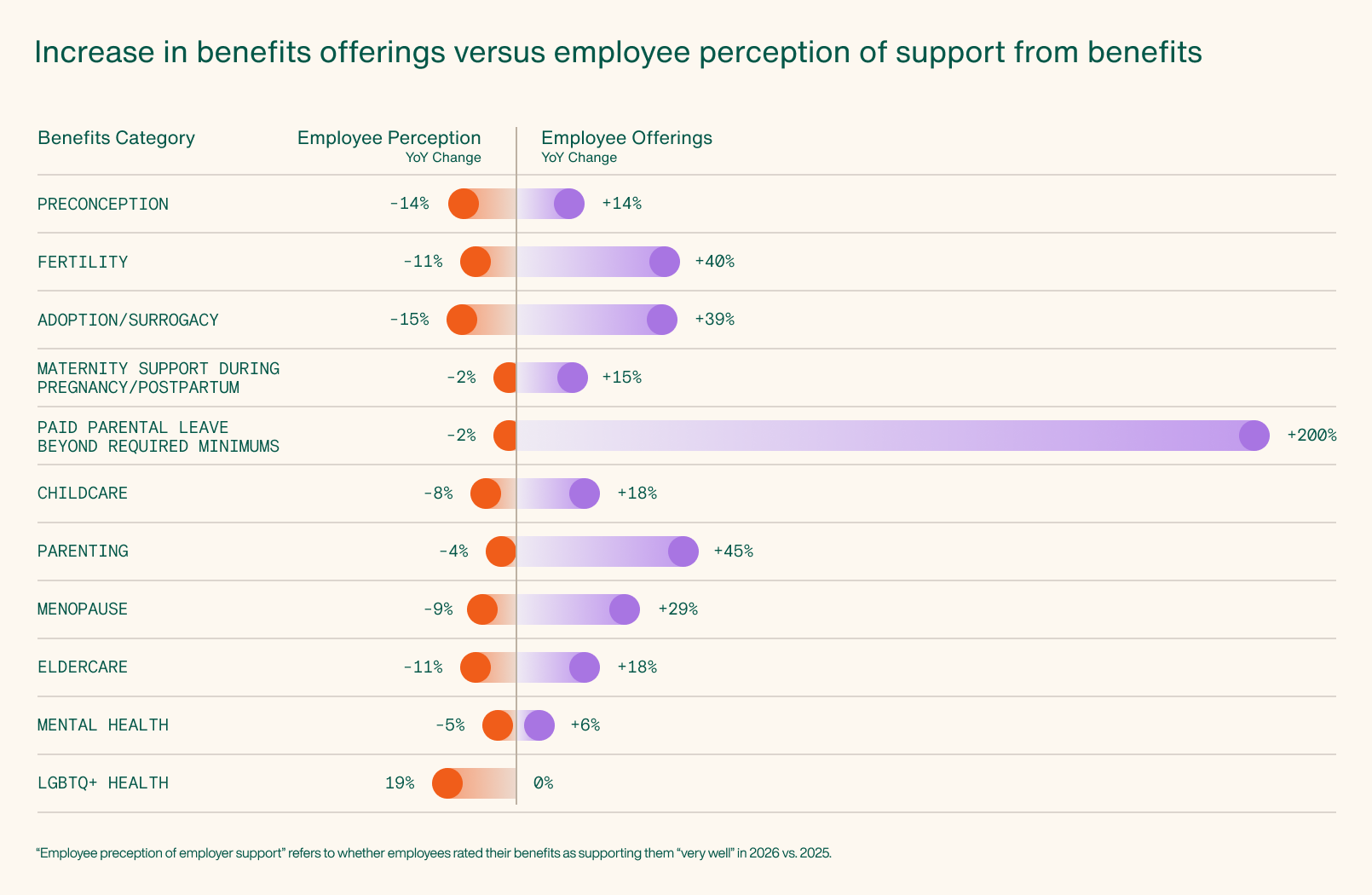
On paper, benefit expansion is real. In the last year, employers have continued to add or grow their offering of women’s and family health benefits; maternity support has increased by 15%, adoption and surrogacy support by 39%, fertility support by 40%, and extended paid parental leave by a staggering 200%. This positive change is expected to continue as employers respond to workforce expectations and rising healthcare complexity, with at least 9% planning to provide more benefits in the next 12 months.
Yet employee perception is trending in the opposite direction. Compared to last year, fewer employees say their benefits support preconception, fertility, adoption, surrogacy, or LGBTQ+ family health “very well”, with sentiment towards them decreasing by an average of 10%.
This widening difference between employer intent and employee experience spans the entire women’s and family health journey. If left unaddressed, this perception gap could damage employee well-being, retention, and equity.
What is driving the employee benefits perception gap?
Fragmentation across vendors
Many organizations now offer a growing number of specialized solutions to their workforce, with 61% of employers expecting to add even more vendors over the next 2-3 years. But while each may address a specific need, employees often have no clear starting place and must navigate multiple platforms, providers, and support lines on their own, often during highly stressful experiences such as infertility or complicated pregnancies.
Communication and navigation gaps
Even when strong benefits exist, employees don’t always have a clear understanding of what is covered, eligibility requirements, how to access care, or where to get assistance. Many benefit leaders say employee engagement and education are the least challenging part of the process, yet only 7% of people turn to employer-provided resources first when addressing a health concern.
Lack of results-driven data
Less than half HR leaders say most or all of their women’s and family health benefit vendors share data. Many employers regularly expand their benefits offering without a clear understanding of the outcomes and impact of current programs, making it difficult to establish what is most beneficial to employees.
How does poor benefits navigation affect employee health and business outcomes?
When employees struggle to understand or use their benefits, the impact extends beyond frustration. Family-building and women’s health journeys are already emotionally complex, and without clear guidance, employees may delay fertility care, postpone other critical care like menopause or postpartum mental health support, or forgo help entirely, increasing the risk of negative health outcomes. Others turn to external resources or out-of-pocket solutions rather than using employer-sponsored programs. Over time, this can increase stress, worsen health outcomes, and reduce trust in the employer.
For employers, this represents not only a human challenge but also a financial one. Research links supportive health benefits with improved engagement and retention outcomes, meaning that when employees can’t access or trust the benefits provided, organizations risk higher turnover, lower morale, and underutilization of costly programs.
How employers can turn benefits into real support
Closing the perception gap requires a shift in focus from the number of benefits offered to how those benefits are experienced. The traditional approach focused on adding more programs to address specific needs—but the future of employee benefits lies in coordinated care, simplified access, and helping employees navigate complex systems with confidence.
This means prioritizing benefit quality over quantity, usability over eligibility, and experiences that build trust rather than simply expanding coverage lists. When benefits are easier to access and understand, employees are more likely to engage with care early and feel supported by their employer.
Collate and consider employee feedback
Employers should identify the challenges their workforce faces when finding or using current support, particularly at crucial moments such as connecting with human support and care or applying for financial reimbursements. Employee feedback is also imperative to understanding where specific improvements are needed, be it in communication or navigating the breadth of providers.
Design a clear entry point into care
Employees need a clear entry point into care rather than a long list of separate programs. They benefit from proactive guidance that helps them understand their options and next steps. Continuity across life stages also matters, since needs often evolve from preconception to fertility, maternity, parenting, midlife, and beyond.
Integrate mental health into family benefits
Given that the stress levels of a woman diagnosed with infertility are similar to those of a woman with cancer, providing mental health support to support a family building journey is critical. Many family health journeys are emotionally complex, and separating emotional care from clinical care can make the experience feel disjointed.
Prioritize inclusivity
Finally, inclusive design is essential. In the US alone, 2.57 million LGBTQ+ adults are raising children under the age of 18, and single-parent households continue to rise. Benefits should reflect diverse family structures and paths to parenthood, including LGBTQ+ employees, single parents, and those using donor services, adoption, or surrogacy.
How Maven helps employers turn benefits into real support
Offering more benefits is only part of the solution. Employees need benefits that are coordinated, understandable, and connected across life stages. Maven helps employers move from a collection of programs to a cohesive care experience that supports women’s and family health from preconception through parenthood and beyond.
Our clinically managed model connects fertility, maternity, parenting, and menopause support within one platform. Rather than leaving employees to navigate multiple vendors, coverage rules, and care transitions on their own, Maven provides structured guidance and continuity at every point in the journey.
What sets Maven apart is the integration of clinical care, emotional support, and benefits navigation. Employees gain access to specialized clinicians and evidence-based guidance that helps them understand their options, make informed decisions, and access the right level of care at the right time.
For employers, this coordinated model helps close the perception gap while delivering measurable impact. Instead of benefits existing only on paper, employees experience connected, personalized support that builds trust and encourages early engagement. This shift is both experiential and financial: employers implementing Maven’s Managed Benefit program see an average of $9,600 savings per birth whilst 47% of members with severe menopause symptoms are more likely to stay with their current employer due to Maven. By aligning navigation, clinical guidance, and benefit design, organizations can drive stronger utilization, better health outcomes, and a more predictable return on benefits spend.
As workforce expectations evolve and healthcare complexity grows, women’s and family health can no longer be treated as separate point solutions. An end-to-end approach helps employers deliver benefits that employees can actually find, trust, and use.
Explore the full State of Women’s and Family Health Benefits 2026 report to learn how leading employers are closing the perception gap, or join the webinar on March 19 to hear industry leaders discuss how to address these trends in workplace benefits.
Ready to get started with Maven?
See how Maven can support working families, retain talent, and reduce costs







.jpg)
.jpg)

.jpg)
.jpg)


