Maven’s latest report found that employees are increasingly using AI tools to inform health decisions, often before engaging with employer-sponsored benefits. While employers remain highly trusted sources of health information, they are rarely employees’ first stop.
- 59% of employees use AI daily or weekly to find health information
- 40% report taking action based on AI-generated recommendations
- Only 7% of employees turn to employer resources first
- Clinically guided platforms like Maven help align convenience with clinical credibility
Artificial intelligence has rapidly shifted from an emerging technology to an everyday tool. Over 60% of American adults used AI in 2025, with one in five relying on it daily. This is particularly pronounced for employed adults, higher earners, and younger employees—groups adopting AI into routine decision-making at a much faster rate.
Healthcare is increasingly part of this shift. Individuals are using AI tools to interpret symptoms, explore treatment options, and answer medical questions. And within the workplace, this behavioral evolution is reshaping how employees engage with employer-provided health resources.
Employees today operate within an information environment defined by algorithm-driven content, targeted advertising, social media, and AI-generated responses. While information has become more accessible, clarity and clinical reliability have not necessarily kept pace. Maven’s State of Women’s and Family Health Benefits 2026 report highlights a significant trend: employees are increasingly turning to AI tools for health guidance long before engaging with employer-sponsored benefits.
Evidently, the shift in employee behavior presents a structural challenge for HR leaders. Trust in employer-provided benefits remains high, yet their actions suggest employees are prioritizing immediacy and convenience when seeking answers.
AI is already shaping employee health decisions
AI adoption within health information seeking is no longer occasional—it is habitual.
Maven’s 2026 research shows that 81% of employees have used AI to find health information, with over half doing so daily or weekly. This reflects a fundamental shift in how individuals approach questions about their health, moving from provider-led resources and traditional search engines toward conversational AI platforms that deliver rapid, simplified responses.

Crucially, this engagement extends beyond passive information gathering. 33% of employees report taking action on their health based on AI-generated information, including scheduling doctor’s appointments and starting or stopping medication. These tools are not simply influencing awareness; they are actively shaping employee behavior.
Employees are responding to speed, accessibility, and reduced cognitive effort. AI platforms offer immediate answers in simple, easy-to-digest formats that often feel easier to navigate than traditional benefit programs.
The employer trust and engagement disconnect: why employees default to AI tools
Despite rising reliance on AI, employees continue to view employers as reliable sources of health information. However, this credibility alone does not automatically translate into behavior. Only 7% of employees report turning to employer-provided resources first when faced with a health-related question. Meanwhile, a third turn to the internet or AI.

At the same time, 51% of HR leaders believe employees primarily rely on employer-provided health platforms for guidance. This difference reveals a clear and persistent perception gap.
Employees are not actively rejecting employer resources; they clearly value their worth. Instead, they are responding to friction. AI tools provide immediate responses, simplified explanations, and interfaces that minimize effort. By contrast, many benefits programs remain fragmented across multiple vendors, portals, eligibility rules, and administrative processes. When employees face urgent or stressful health decisions, navigating benefits systems can feel slow or complicated—particularly when compared to the conversational ease of AI.
The challenge for employers is not centered around credibility, but instead accessibility, usability and engagement.
The risks of unmanaged AI-driven care decisions
While AI platforms offer convenience, they do not guarantee clinical accuracy or safe care pathways.
A major new study from the University of Oxford has confirmed that LLM chatbots pose real risks when giving medical advice. In a randomized trial of nearly 1,300 participants, researchers found that various LLM models correctly identified medical conditions and appropriate next steps less than half the time—a performance level comparable to traditional internet searches.
The findings suggest that while AI models may perform well in controlled environments, their responses in practical health-seeking scenarios can be inconsistent or misleading, reinforcing the need for human oversight. Even actions such as changing medication or self-managing symptoms can result in missed early intervention, as well as higher costs to employee wellbeing and employer healthcare spend.
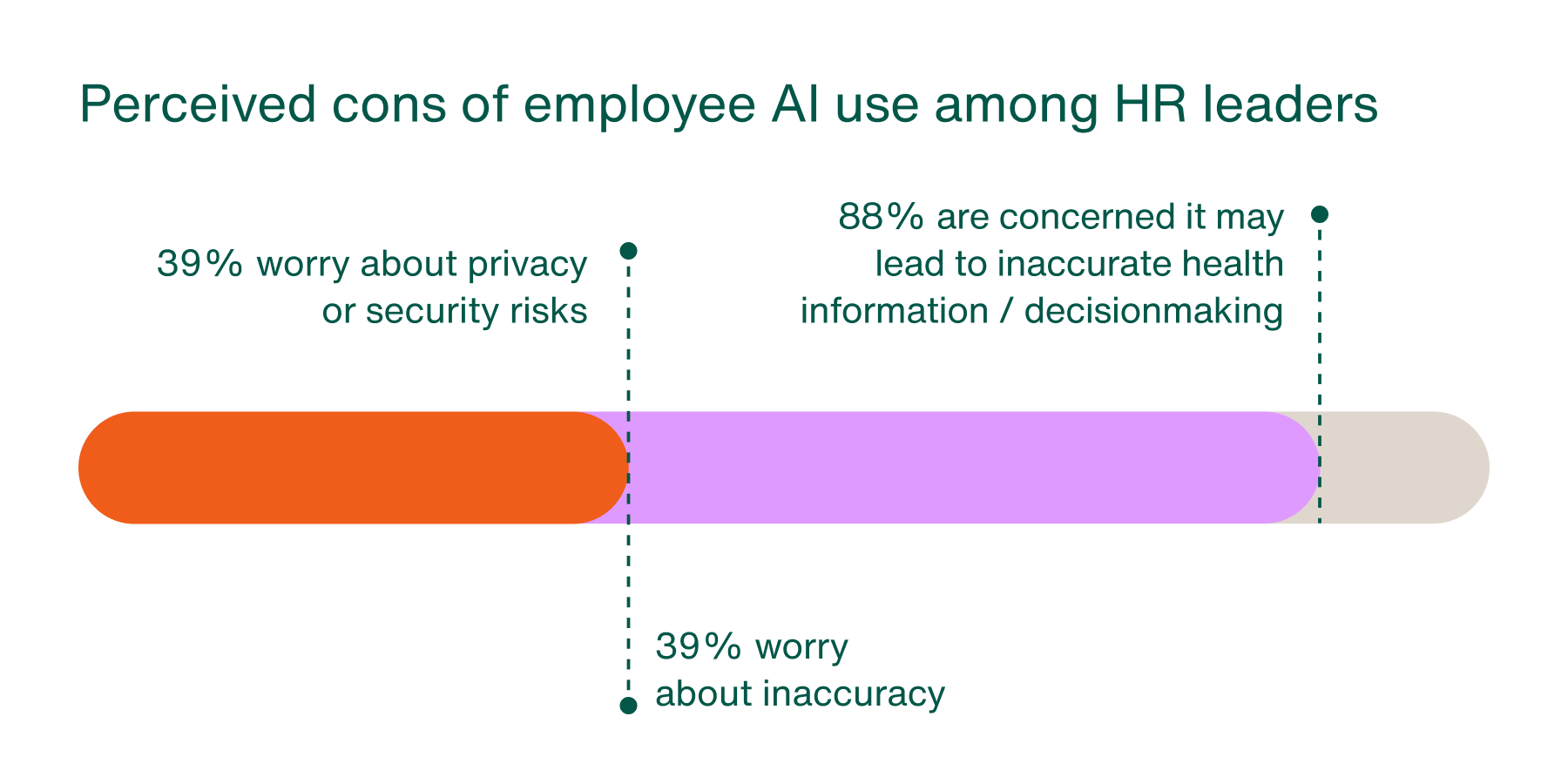
Employers are generally in agreement, with 9 in 10 HR leaders expressing concern that employees may make decisions based on inaccurate or incomplete guidance from AI tools.
Data privacy considerations further complicate this issue. Many consumer AI platforms are not designed to manage protected health information within healthcare-specific regulatory frameworks. Employees may unknowingly share sensitive medical data with AI tools that are not designed to protect it, creating potential compliance and privacy risks for organizations.
The opportunity and potential of AI within benefit programs
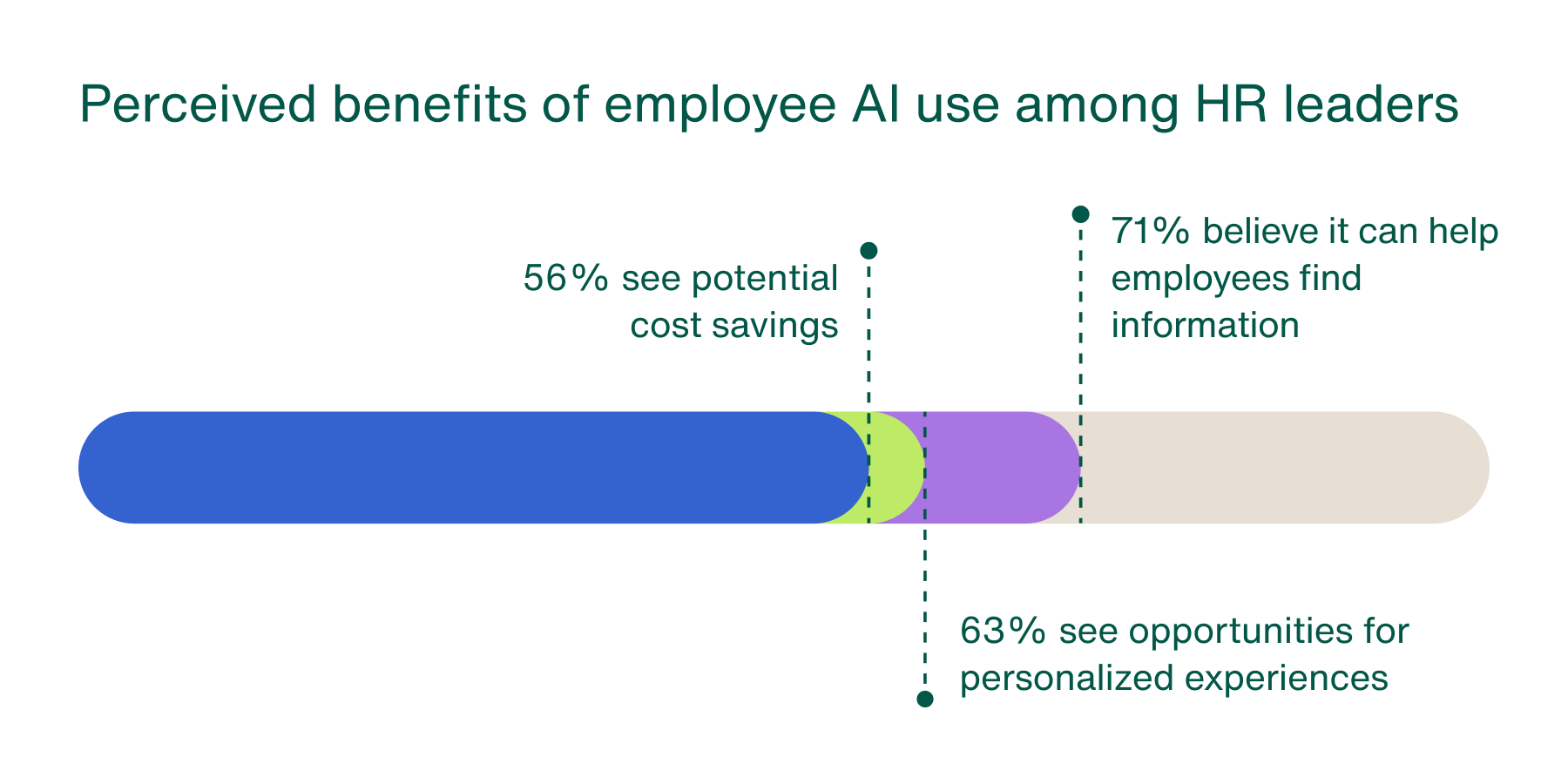
AI use in health decision-making signals a broader shift in how employees seek information, not a passing trend. While many HR leaders express concern about employees acting on inaccurate AI-generated guidance, most recognize its potential. Over 71% of HR leaders believe AI can help employees find information more quickly and easily, 63% see opportunities to improve personalization and efficiency, and more than half believe AI could contribute to cost savings.
This duality reflects a significant turning point for benefits strategy. Employees are not rejecting employer-sponsored benefits; they are prioritizing speed, clarity, and convenience. For employers, this reshapes the challenge. Benefits are no longer evaluated solely on what they cover but on how easily employees can access guidance and support. Rather than competing with AI, benefits strategies must evolve alongside it.
How HR leaders can respond to increased AI adoption
- Provide a trusted first stop. Employees often default to AI because it is immediate and frictionless. Employers can counterbalance this by making it unmistakably clear where reliable health guidance lives within the benefits ecosystem.
- Balance accuracy with convenience. Speed is valuable but without clinical oversight, it introduces risk. Partnering with solutions that combine digital accessibility with evidence-based medical guidance helps employees access answers quickly while protecting safety, privacy, and outcomes.
- Embed navigation into care pathways. Health decisions rarely happen in isolation. Benefits work best when education, guidance, and care navigation are delivered through a connected experience rather than spread across multiple tools.
- Communicate proactively, not reactively. Employees regularly consult AI when uncertainty arises. Regular, life-stage-specific education (such as menopause) helps establish employer resources as a natural reference point before critical decisions are made.
By aligning convenience with clinical oversight, employers can reduce unmanaged decision-making, improve benefits utilization, and reinforce trust within an increasingly AI-driven health landscape.
How Maven helps employers guide employees in an AI-driven health landscape
As employees increasingly turn to AI for immediate answers, employers face a new benefits challenge: ensuring convenience does not come at the expense of clinical accuracy, safety, or trust.
Maven helps organizations meet this need through a clinically grounded, end-to-end care model. Rather than relying on fragmented vendors, employees gain access to a user-friendly platform access to 24/7 virtual care and support across fertility, maternity, parenting, and menopause and midlife health. This structure supports the need for immediacy while maintaining the clinical oversight, coordination, and data security required for sensitive health decisions.
Importantly, Maven does not position AI as a replacement for care, but as a tool that strengthens care delivery by helping members access the right support, faster. Members can engage with Maven Intelligence as a seamless front door to care on Maven, similar to how they might use a generic AI tool. Unlike these generic models, however, Maven Intelligence is purpose-built for women’s and family health and trained on a decade of real-life experience supporting women’s and family health. Behind the scenes, Maven Intelligence draws on a member’s history, goals, benefits coverage and integrated data — including EHR records, lab results, and wearable inputs — to surface personalized, evidence-based guidance, connect members to the appropriate providers, navigate benefits and reimbursement pathways, and prompt follow-up when needed. These tools operate within a secure, healthcare-grade environment designed to protect privacy while improving care experiences and outcomes.
For employers, this coordinated approach helps reinforce trusted care pathways, improve benefits utilization, and translate health investments into more measurable outcomes. Those who invest in Maven see up to $9,600 per member in combined clinical and business savings, with total savings reaching up to four times program costs.
Explore the full State of Women’s and Family Health Benefits 2026 report to learn more about how AI is reshaping employee health decision-making, or book a demo and see how Maven can work for your organization today.
Ready to get started with Maven?
See how Maven can support working families, retain talent, and reduce costs



.jpg)

.jpg)


.png)
.png)

.png)
.png)
.png)
